Public health may not always benefit you...but that doesn't matter
As an epidemiologist and public health researcher, I'm often asked my opinion on timely health-related topics. Example questions include:
From a friend few years back, "Will Zika affect my pregnancy?" Me: probably not, as we live in a state without local transmission of the virus, and this couple had not traveled to any high-risk areas.
From my parents last Fall, "Should I get a flu shot this season?" Me: sure, although the vaccine may not completely cover the circulating strains, it's always a good idea especially among those 65 years of age and older.
From the media during interviews on the coronavirus pandemic, "Should face masks be required in public? Should schools reopen in the Fall?" Me: Pull up a comfortable chair because these are not simple yes or no answers, and the science is constantly evolving. What I tell you today possibly will not be the case tomorrow.

What is inherent in all these answers is an acknowledged level of uncertainty. Note the use of words "probably," "may," and "possibly." It's not that public health professionals are trained to be deliberately ambiguous, but science and its evidence are constantly evolving, and answers such as these provide a certain amount of semantic wiggle room necessary to convey this uncertainty.
What is public health?
Before delving further into this uncertainty, as a professor, I need to be clear about key terms. Public health is literally the health of populations of people. What is health? It's not only being free of diseases. It is as defined by the World Health Organization as a state of complete physical, mental, and social well-being. A population may be your town or city (local health departments), an entire state (state health departments), or even the entire country (the Centers for Disease Control and Prevention). Care is not provided on a per-person basis as would occur from a physician in a clinical setting, but rather through interventions like policy and public service announcements. Such achievements include mandatory vaccination requirements upon school entry for children, seatbelt laws, recommendations for diet and exercise, smoking cessation interventions, safe sex campaigns, screening for cancers, social distancing and shelter in place orders during a pandemic, and so on. The hope is by having enough people engage in these advised behaviors and lifestyles the overall population will be healthier.
The trouble is, not everyone has agency or desire to make a change and some factors may be immutable, such as family history of disease or the aging process.
How can we measure the public's health? One way is through markers, such as infant mortality and life expectancy. In fact, in the twentieth century life expectancy increased an average of 30 years; a truly remarkable feat of which much of the increase was attributable to public health interventions!
Does this mean that each and every individual born at the end of the twentieth century lived exactly 30 years longer than previous generations born at the start of the century? Of course not, but now we begin to see a certain paradox that arises from the way public health measures are conveyed: what happens at a population level may not be a marker for what happens at the individual level. From an ethics standpoint, public health typically operates under a utilitarianism perspective: the greatest good for the greatest number. Therein lies the tension.

Individual versus public health
This is not a new concept: a seminal paper discussed sick populations versus sick individuals in 1985. When a sick patient seeks guidance and treatment from a physician, often the physician will couch the therapy by saying "In most people, we will expect to see..." It is clear from this statement that "most people" implies some population where the therapy was tested and it may not exactly translate to you as the individual.
Let's take a public health example: smoking cessation interventions. We have all seen the copious warnings on tobacco products, public service advertisements on television and billboards, and brilliant social media campaigns by organizations such as Truth. The message is elegant in its simplicity: if you smoke, you are at increased risk for disease and death. This is easily measurable at a population level, and research studies are available from as far back as the 1950s indicating this elevated risk. So why does it seem we all have a George Burns in our family, who smoked like the proverbial chimney and lived an exceedingly long life?
This is where we begin to see how a population intervention may not benefit a given person. The irony to this is as epidemiologists, we are trained to be as precise as possible in measuring the risks associated with a behavior or condition, but when we go to disseminate the results, we use imprecise language acknowledging this reality. We may be able to measure a risk increase in lung cancer associated with smoking as 83.357% (+/- 3.25%) that of a nonsmoker, but when you see the warning label on the pack of cigarettes, it clearly states, "This product may cause lung cancer," (emphasis added), not "This product causes lung cancer in 83.357% of smokers."
As another and more debated example, we can turn to childhood vaccination. The science is unambiguous and definitive: vaccines work. They have minimal risk and maximal benefit. Public health authorities have emphasized this message for decades. Parents choosing not to vaccinate may be lulled into a false sense of security as the childhood diseases, like measles and diphtheria, we vaccinate against are pretty rare. [Even the measles outbreak of 2019 is still by definition rare at a population level]. As an epidemiologist, I can never categorically state that a child whose parents opted out of vaccination will get measles, particularly if the community where this family resides is otherwise well vaccinated, a phenomenon known as community immunity. This child is certainly much more likely than their vaccinated peers, but it is not a dichotomy. Conversely, I can also never categorically state that the parent who vaccinates their child with all recommended doses will not get measles or diphtheria. It is exceedingly rare, but sadly it does happen. Vaccines are not perfect and not without risks, however exceedingly small. For the parent who rightfully chooses to vaccinate their child, public health may let them down in the rare case the child becomes ill or suffers a severe adverse reaction.
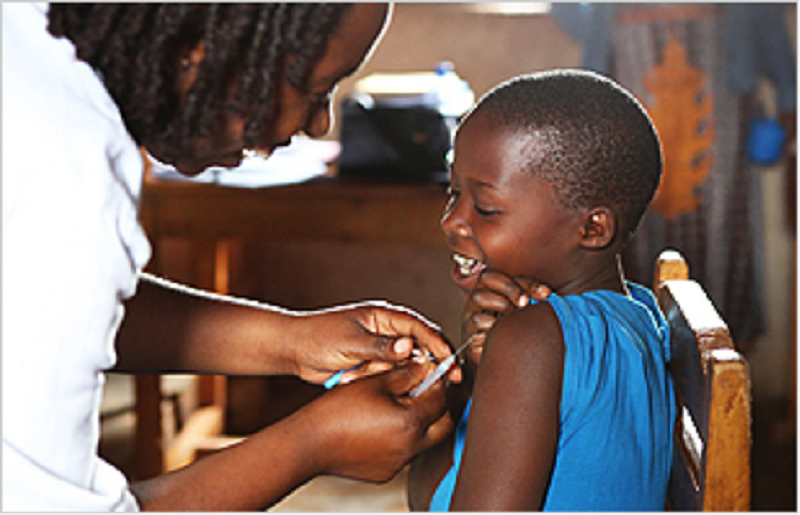
We have no way of knowing with complete certainty which public health interventions will benefit which individuals. There is some notion of altruism at play as well. If I do something that may not directly benefit me, I hope that it benefits someone else. A lot of public health threats, particularly infectious disease ones including most sexually transmitted infections, are well studied and the interventions well known. Even if I choose to wear a condom during sex, I may be putting my partner at risk because condoms are not perfect. If I choose to not wear a mask to prevent spread of coronavirus, I may be comfortable with my risk of being exposed, but I am potentially putting other people at risk if in fact I am asymptomatically infected.
Epidemiologists provide the evidence at a population level of these interventions. I hope that individuals choose to use vaccines, condoms, quit (or never start) smoking, and otherwise follow the guidance from public health authorities, but I also recognize that these interventions are not fool-proof, and the individual who gets vaccinated, uses a condom, and never smokes may come down with whooping cough, have an unintended pregnancy, and die of lung cancer.
There is also a breadth of articles in scholarly literature discussing the tension between public health interventions and the role of individual choice. Certainly I cannot legislate that having sex without a condom is illegal [although HIV criminalization laws have been infamously tried], but public health has many policies that are the result of legislation, such as school vaccination requirements. In these cases where public health policy is the result of legislation, the public's welfare needs to override the individual's liberty to abstain from these interventions. Court cases that challenge these laws as a violation of Constitutional rights usually fail because these laws do not differentially impact any class or group of individuals and the overriding public interest of keeping the population healthy is paramount.
Challenges faced by public health
Returning to a point made earlier, individuals do not always have agency, incentive, or desire to listen to public health recommendations. Perhaps these individuals recognize that a one-size-fits-all approach may not benefit them, would like to change but can't, or view public health as a real threat to their autonomy in decision making, the familiar battle cry of keep the government out of my health. The ability to change is not always an onus placed on individuals. As we say in public health, place matters. Smoking is exceedingly difficult to give up when you are surrounded by other smokers. Living in an impoverished neighborhood or being forced to leave your existing neighborhood due to elevated costs of living associated with gentrification often results from a lack of autonomy and agency, perhaps as a result of systematic policies of oppression, such as the practice of "redlining." Again, when we turn to the literature, we see that individuals who move frequently or live in a neighborhood below the federal poverty line have worse health than do counterparts in stable housing in a more affluent area. Public health interventions that improve the neighborhood, such as building more parks or a community garden, may face challenges if those parks turn into areas of crime or drug sales and use.
We also have to acknowledge the potentially fickle nature of public health. Not only must an area be exceedingly devastated with a health problem, it most garner widespread attention before individuals gain agency. Post Hurricane Katrina, the Flint Michigan water crisis, and now in the storm of the pandemic, the initial response was underwhelming, and it was not until local organizations pushed through to the national spotlight that additional relief efforts became available. Many suffered and died during this time: a failing of public health [I do not wish to implicate the entire field, as grassroots efforts mobilized tremendous resources in a short time]. And perhaps this failing has led to a further rift and distrust between individuals and public health authorities.
Public health and science are fallible
The reality is public health is not a panacea to societal health. It represents our best knowledge about disease and other health conditions at a point in time. This changes as society and the science evolve. As has been said before, the hallmark of a good [public health] scientist is someone who is willing to change their mind. At one point, science suggested that hormone replacement therapy in postmenopausal women may have been beneficial to reduce risk of heart disease. Then the Women's Health Initiative found it was harmful in that women had an increased risk of certain cancers. Now we seem to think it may be beneficial again, but only within a certain segment of the population of women, namely those perimenopausal and for a short duration of therapy.
As another example, public health messaging has largely shifted from fear-based negative ads to positive ads over the last few decades. Towards the beginning of the HIV/AIDS epidemic, public health ads were often critiqued as fear-based and potentially stigmatizing. It was argued that these ads further exacerbated an already stigmatizing condition, and that this stigma could lead to adverse health outcomes.

A host of recent studies have called to question many scientific findings as lacking reproducibility. But this does not mean we should abandon progress, defund science, or further public distrust in scientific findings. There's nostalgia for the past among certain people, a desire for simpler times. This is not admirable from a health perspective. Science is self-correcting over time. We should not discard the advances of the previous century because public health does not always benefit the individual.
How scientific studies can lead to inconsistent evidence
To summarize, public health is a population measure of health indicators that do not necessarily equate to an individual's risk. But why? Well, to answer this question, we first need to become epidemiologists and conduct a study. Our hypothetical research question will be the one I was asked by my parents, "Should I get a flu shot this season?" For a flu vaccine to be licensed for use in patients it must undergo thorough and rigorous scientific evaluation, ultimately approved by the Food and Drug Administration for sale in the U.S. Under the evidence-based medicine paradigm - scientific data is dogma for patient care - a randomized controlled trial must be conducted to establish the efficacy of the flu vaccine. In this trial, the vaccine will be compared to placebo, or an inert compound. Given that we already have efficacious flu vaccines, a placebo comparison may not be ethical, but for the purposes of this hypothetical, we will assume there are no existing vaccines. This trial is undertaken in a group of participants, the vaccine is administered to some, and they are followed over the ensuing year to see who caught the flu.
We can reasonably expect in the group of participants in this trial, some of which who received vaccine and others placebo, that a proportion of people within each group will catch the flu. In advance, we hypothesize the proportion will be greater in the placebo group, but still expect nominal numbers in the vaccine group. Importantly, as the data are analyzed, the outcome measure becomes an average of each group's effects. In other words, the aggregated data trumps the individual effect. Consequently, the vaccine may demonstrate efficacy in the majority, but have a minority who did not benefit, or worse, were harmed. This is also the essence of public health. Why did we not see an effect in certain people who were vaccinated, or see protection in people who were not vaccinated? It may have to do with individual genetics, their social networks (having contact with someone who is infected), low level disease that was not diagnosed, or other myriad factors. Further, in this type of trial, the population recruited to participate is fairly contrived in that only certain types of people actually participate. It is well known in the research world that clinical trials often fail to adequately include minority groups.
In contrast to this contrived clinical trial, under a paradigm known as reality-based medicine, we may observationally follow a group of people in the real-world. As investigators we do not manipulate who was vaccinated and who was not, rather we allowed people to naturally select vaccination, as occurs in society outside of the experimental model. [Although I suggest that people naturally select flu vaccination, this may be related to employment policies, school requirements, or other external forces. By naturally selected, I therefore only imply that the study investigators did not influence receipt of the flu vaccine among study participants.] This reality-based medicine paradigm may be preferred evidence as to the public health benefits from vaccination, because ideally we want people to voluntarily choose a public health intervention, not be coerced into it. Yet as compared to the randomized clinical trial (experimental study), under this observational study we are likely to see differing performance from the vaccine. Individuals who choose to be vaccinated likely engage in other health behaviors and are thus are at lower risk of acquiring infectious diseases. The data are aggregated as before to arrive at population level estimates.

Importantly, under both paradigms, the studies show that vaccination works in some proportion of people implying that in some other proportion of people (presumably the minority) the vaccine did not work. If the signal from the vaccinated group is strong enough, that is, if the vaccine appeared to confer adequate protection with minimal risks, the vaccine will be licensed for use and promoted as a tool in the public health toolbox.
Let me be clear: from the public health perspective, the vaccine works. Once real-world data are aggregated together from the last flu season, there will be demonstrable evidence that among those who chose vaccination there were fewer cases of flu. Further, for those vaccinated who got sick, the intensity and course of the disease may be minimized. From the individual perspective, the effectiveness of the vaccine depends upon in some part how similar you are to the people under study from the clinical trial and in some part how similar you are to the people from the real-world observational study. There may be a preponderance of evidence to suggest you will be protected after vaccination but there is no guarantee. As the adage goes, only death is ensured in life [or at least as of this writing it was!].
Who benefits from population health?
Most public health programs are built around large populations being affected by disease. Before smoking cessation campaigns scaled up, lung cancer was a leading cause of death in the U.S. and abroad. At any given point in time, visiting your local health department's website will yield the most pressing public health concerns in your area. But what if you are affected by an infrequent or downright rare disease, such as a prion disease such as Creutzfeldt-Jakob disease [think mad cow disease in humans]? Under this hypothetical, public health has little to offer you: you become a statistic in the annual health report as the "count" of a reportable disease condition: the one in a million case. These surveillance efforts are useful to direct the health department allocation of funding, and in this case, direct the funding from exceedingly rare conditions to common, prevalent conditions. Perhaps we'll never know how Creutzfeldt-Jakob disease arose in this individual [can you get it from tainted meat?]. As stated earlier, this is the utilitarian paradigm that public health operates under: for the good of the many. The corollary to this is the few will not benefit from public health, and as suggested earlier, a public health intervention may not avail itself until too late.
Now that I have potentially instilled doubt into your mind about the data used in public health, I would like to spend the last part of this essay to allay this concern. First, you are most likely the average person. Unlike what your mother may have told you, you probably are neither special nor unique [sorry!]. But this is a good thing, because if public health interventions are built around the average population effect, being the average individual will yield direct and tangible benefit. Although your Uncle Burns smoked his whole life without cancer, you are likely to be the person who develops cancer, a metabolic or cardiovascular disease, therefore quitting smoking will benefit. Or better yet, by never starting to smoke you are probably not going to get lung cancer. You're likely not to get a sexually transmitted infection if you avail yourself of safe-sex practices. Again, being average works!
Second, even if you are the unlucky individual affected with a health issue [your mother was right: you are special and unique...sorry!], being in a healthier community will increase your access to resources and availability of care, improve your prognosis, and reduce disease effects and adverse outcomes. Further suppose, unfortunately, you decide to abstain from one of the most remarkable public health achievements: vaccination. Living in a community with an overall high proportion of individuals vaccinated may still protect you from disease. Trouble is, people who tend to abstain from vaccination tend to cluster together due to homophily, but that is another topic altogether. The point is place matters.
Third and last, and to quote a recent book of the same name, having less medicine may yield more health. [I wish I could take credit for this provocative and straightforward title, but credit belongs to H. Gilbert Welch, author of the book Less Medicine, More Health: 7 Assumptions That Drive Too Much Medical Care] Some public health interventions, such as population screening for diseases like breast and colon cancers, have a downside to them. The downside is, once you enter the healthcare arena, you are likely to have a health problem found. This often results in unnecessary procedures, with all subsequent risk, monetary expenditure to the healthcare system, and the stress and anxiety of having a false positive finding on one of these screening tests. [A false positive means the screening test showed something of potential interest, but it later turned out to be benign]. I am not suggesting that we turn away from these services, but we need to recognize they are fallible and perhaps use them more judiciously. Sometimes screening tests will miss disease, but they may also find disease when there really isn't any. And if they do find a disease, say a cancer, some cancers are so slow progressing and of little harm, that the intervention itself may be comparatively worse.
We are all individuals as well as members of a community
For those who embark on a career in medicine, you will be focused on individual, patient-specific outcomes. For those who work in public health, you're focus is on populations, not individuals. A famous professor of epidemiology, Mervyn Susser, sought to bridge the two worlds when he wrote that "[d]espite the epidemiologist's insistence on studying populations, his ultimate concern is with health, disease, and death as it occurs in individuals" [Causal Thinking in the Health Sciences, p59]. When discrepancies between the two arise, the interplay between the individual and community may not be immediately apparent. As an example, we can turn to the current debate surrounding face masks for prevention of coronavirus infection. An individual may be willing to take on a greater risk by not wearing a mask. However, if this individual is placed in a setting that has a high likelihood of exposure, such as in a healthcare environment, they may place others at risk through asymptomatic transmission (if the individual were infected but did not realize it) or they may become infected and pass on the infection to others. As another example we can consider motorcycle helmet laws. While some may maintain this decision only affects themselves, and they are willing to take the risk, there are downstream community implications of this decision. Should this individual be injured while riding, there are potentially substantial costs incurred to the healthcare and insurance systems, where risk is managed through pools of individuals (i.e. a community).

Public health strives to do more good than harm, and is largely responsible for the increased length of life that many of us will enjoy. This essay has hopefully revealed that there is both an art and science to the approach of this discipline, and that sometimes public health professionals need to make difficult decisions despite scientific uncertainty. By recognizing these limitations of public health, we can all be better consumers of health.
Cite: Goldstein ND. Public health may not always benefit you...but that doesn't matter. Aug 5, 2020. DOI: 10.17918/goldsteinepi.